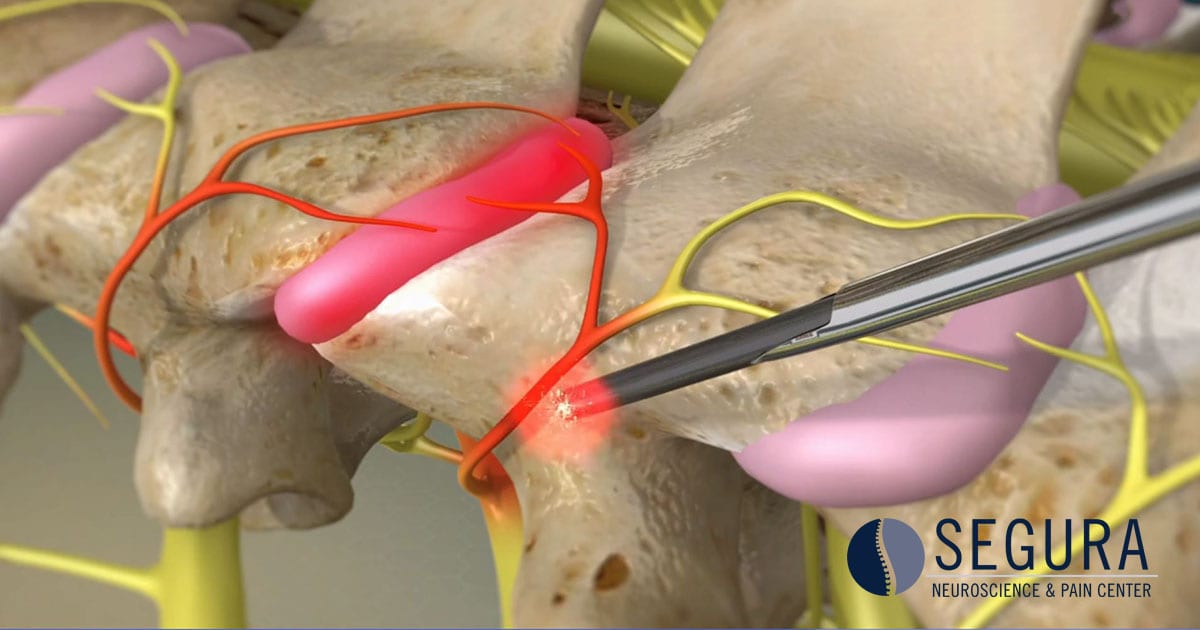
Radiofrequency ablation (RFA) is a minimally invasive procedure designed to reduce or eliminate pain through the application of heat. In this procedure, an electrical current is used to burn problematic nerves, preventing them from sending pain signals. RFA may be used in patients suffering from chronic pain.
Who can benefit from RFA?
Conditions causing inflammation, specifically in facet and sacroiliac joints, can be treated with RFA. Patients who have achieved successful pain relief after a diagnostic nerve block injection may be good candidates for this procedure. Patients suffering from pelvic pain or neck and back conditions like spondylosis may also find relief after radiofrequency ablation. RFA can also successfully treat shoulder and knee pain, occipital neuralgia, and certain types of headaches.
What does the procedure entail?
 The procedure begins with the patient lying on their stomach. If the patient requires sedation, an intravenous (IV) tube is inserted to administer medication. The physician then numbs the procedure site by injecting an anesthetic under the skin. Using real-time x-ray guidance (fluoroscopy), the RFA needle is guided toward the affected nerves. Once the nerve is located, a small active current is passed through the needle to briefly recreate the pain typically experienced by the patient, confirming that the correct nerve has been located. A heat lesion is then placed on the nerve, blocking it from sending pain receptors to the brain.
The procedure begins with the patient lying on their stomach. If the patient requires sedation, an intravenous (IV) tube is inserted to administer medication. The physician then numbs the procedure site by injecting an anesthetic under the skin. Using real-time x-ray guidance (fluoroscopy), the RFA needle is guided toward the affected nerves. Once the nerve is located, a small active current is passed through the needle to briefly recreate the pain typically experienced by the patient, confirming that the correct nerve has been located. A heat lesion is then placed on the nerve, blocking it from sending pain receptors to the brain.
What to expect after the procedure
Radiofrequency ablation typically takes about 30 to 90 minutes. Patients can usually return home the same day but should not drive or do any rigorous activity for 24 hours. Some patients may experience temporary soreness at the incision site, but most are able to return to normal activities the day after the procedure. Results vary between patients, and while many feel relief for 6 to 12 months after radiofrequency ablation, some remain pain-free for years.